The Three-Way Tug-of-War: Calcium, Phosphorus, and PTH
To understand how this happens, you have to look at the relationship between three main players. Normally, your kidneys filter out extra phosphorus. When the Glomerular Filtration Rate (GFR) drops below 60 mL/min, phosphorus starts building up in the blood. This is where the trouble starts. High phosphorus acts like a trigger, pushing calcium out of your bones and into the bloodstream, while simultaneously signaling your parathyroid glands to go into overdrive.
The Parathyroid Glands are four tiny glands in your neck that act as the thermostat for calcium. When they sense low calcium or high phosphorus, they release Parathyroid Hormone (PTH). In CKD, this becomes a permanent state called secondary hyperparathyroidism. The PTH tells your bones to release more calcium to keep the blood levels steady. While this solves the short-term blood calcium problem, it effectively "strips" the minerals from your skeleton, making your bones brittle and porous.
The Vitamin D Connection and the FGF23 Factor
You can't talk about bone health without mentioning Vitamin D. But here is the catch: the vitamin D you get from the sun or a supplement isn't actually "active." Your kidneys are responsible for converting it into calcitriol, the active form that helps your gut absorb calcium. When kidneys fail, calcitriol production plummets-sometimes by as much as 80% in advanced stages.
Adding to the chaos is a hormone called FGF23 (Fibroblast Growth Factor 23). Your body pumps out FGF23 to try and force the kidneys to dump phosphorus. However, FGF23 has a nasty side effect: it further suppresses the production of active vitamin D. This creates a vicious cycle where the body is desperately trying to lower phosphorus but, in doing so, kills off the vitamin D needed to maintain bone strength. This is why about 80-90% of patients in Stage 3-5 CKD suffer from significant vitamin D deficiency.

When Bone Disease Turns Into Vascular Danger
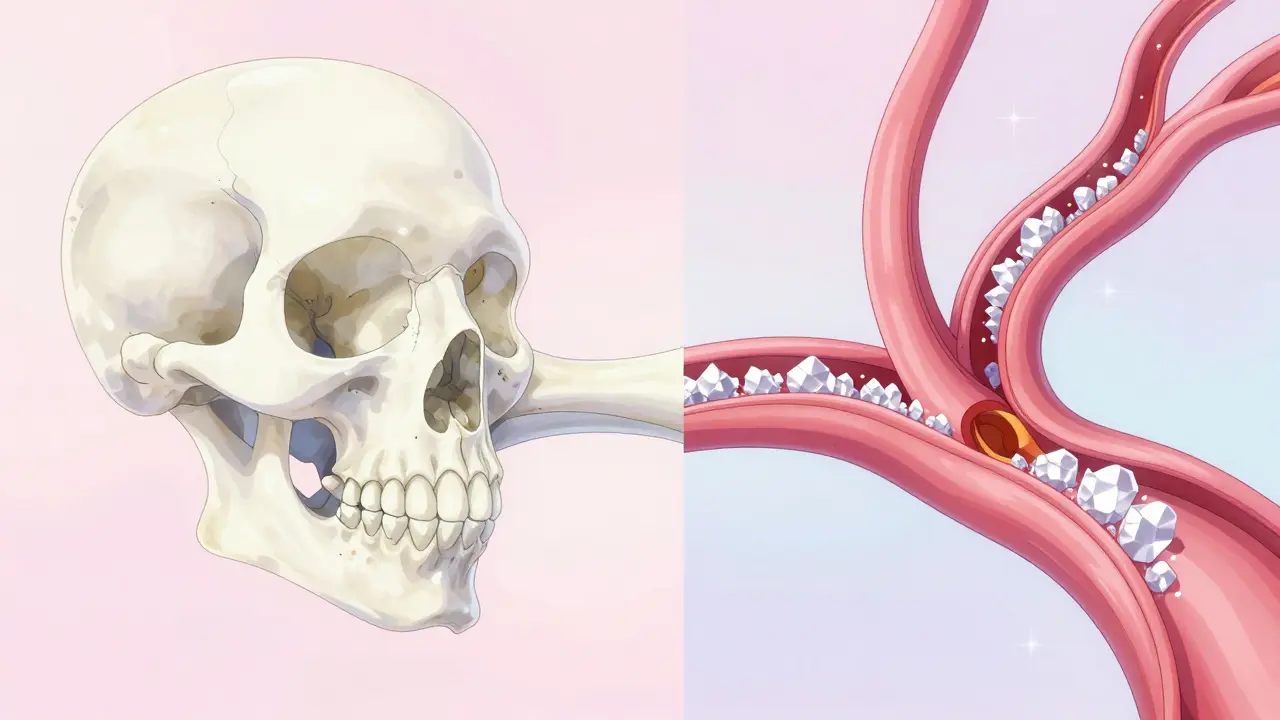
The danger of CKD-MBD isn't just that you might break a bone-though the risk of a hip fracture is 4-5 times higher for dialysis patients than for the general public. The real threat is where that displaced calcium goes. When calcium is stripped from the bone and can't be balanced, it starts to deposit in the soft tissues and blood vessels. This is called Vascular Calcification.
Essentially, your arteries begin to turn into bone. This stiffens the blood vessels, raises blood pressure, and significantly increases the risk of a heart attack. In fact, coronary artery calcification is present in up to 80% of dialysis patients. It's a grim irony: the very minerals meant to make your skeleton strong are instead hardening your heart's plumbing.
| Feature | High Turnover (Osteitis Fibrosa Cystica) | Low Turnover (Adynamic Bone Disease) | Mixed Uremic Osteodystrophy |
|---|---|---|---|
| PTH Levels | Very High (>500 pg/mL) | Low (<150 pg/mL) | Variable |
| Bone Formation | Rapid but disorganized | Very slow/stagnant | Combination of both |
| Fracture Risk | High | High | High |
| Prevalence (Dialysis) | 20-30% | 50-60% | 10-20% |
How Doctors Manage the Mineral Chaos
Managing CKD-MBD is like trying to balance a scale where every adjustment tips something else over. If you lower phosphorus too aggressively, you might trigger malnutrition; if you give too much active vitamin D, you might cause hypercalcemia (too much calcium in the blood), which accelerates heart calcification.
Treatment usually follows these primary paths:
- Phosphate Control: This starts with diet (limiting phosphorus to 800-1000 mg/day). When that's not enough, Phosphate Binders are used. These are medications taken with meals to "bind" phosphorus in the gut so it's excreted rather than absorbed. Common options include sevelamer or lanthanum carbonate. Calcium-based binders are used cautiously because too much elemental calcium (over 1500 mg/day) can worsen vascular calcification.
- Vitamin D Therapy: For simple deficiency, nutritional vitamin D (cholecalciferol) is used. For severe cases of secondary hyperparathyroidism, active analogs like calcitriol are used to trick the parathyroid glands into slowing down.
- Calcimimetics: When PTH levels are dangerously high, drugs like Cinacalcet are used. These drugs fool the parathyroid glands into thinking there is enough calcium in the blood, which drops PTH levels without adding more calcium to the system.
Monitoring and Red Flags
Because this disorder is systemic, you can't rely on how you feel. You can't "feel" your arteries calcifying or your PTH levels climbing. Regular blood work is the only way to stay ahead of the curve. Doctors typically look for a serum calcium level between 8.4 and 10.2 mg/dL and a phosphorus level between 2.7 and 4.6 mg/dL for those in Stages 3-5.
If you are on dialysis, the targets shift slightly, but the goal remains the same: prevent the "bone-to-vessel" mineral shift. While bone biopsies are the gold standard for checking bone turnover, they are rare. Instead, your doctor will use PTH levels and markers like bone-specific alkaline phosphatase to guess what's happening inside your skeleton.
Why is phosphorus so dangerous in kidney disease?
Phosphorus is dangerous because the kidneys can't remove it. When levels rise, it binds to calcium, pulling it out of your bones (making them weak) and depositing it in your blood vessels (making them stiff). This increases your risk of both fractures and heart failure.
Can I just take a standard Vitamin D supplement?
You should only do this under medical supervision. While nutritional vitamin D (cholecalciferol) is often needed, taking active vitamin D (calcitriol) without monitoring can lead to dangerously high calcium and phosphorus levels, which can accelerate the hardening of your arteries.
What are the signs that my bones are affected?
Bone disorder in CKD is often "silent" until a fracture occurs. However, some patients experience bone pain or joint stiffness. Because the risk of fractures is 2.5 to 5 times higher than in the general population, preventative management of PTH and phosphorus is critical.
What is the difference between high and low bone turnover?
High turnover (Osteitis Fibrosa Cystica) happens when very high PTH levels cause bones to break down and rebuild too quickly, creating weak, fibrous bone. Low turnover (Adynamic Bone Disease) occurs when bone activity almost stops entirely, often due to over-suppression of the parathyroid glands. Both increase fracture risk.
Do phosphate binders actually work?
Yes, they are highly effective at preventing phosphorus from entering the bloodstream from the food you eat. However, they must be taken exactly as prescribed-usually right with meals-to be effective. The choice of binder (calcium-based vs. non-calcium) depends on your current calcium levels and vascular health.
Next Steps for Patients and Caregivers
If you're navigating a CKD diagnosis, the first step is to ask your nephrologist for your latest PTH and phosphorus numbers. Don't just ask if they are "normal"; ask where they sit relative to the KDIGO guidelines. If you are in Stage 3, ensure you're getting annual 25-hydroxyvitamin D tests to catch deficiencies early.
For those on dialysis, pay close attention to your binder timing. Taking a binder after you've finished your meal is far less effective than taking it during. Also, keep a food diary to identify hidden phosphorus sources-like processed meats and dark sodas-which often contain additives that are absorbed much more easily than phosphorus found in natural foods.








Srikanth Makineni April 5, 2026
phosphorus binders are the real game changer here
Jay Vernon April 5, 2026
Wow this helps a lot 😊 It is scary how the heart gets affected too 💔 Stay strong everyone! ❤️
Toby Sirois April 6, 2026
Everyone acts like this is new info but any basic med student knows the FGF23 pathway is the real culprit
You just have to manage your diet better if you actually care about your health
Most people just ignore their phosphorus levels until they are in a wheelchair
It is common sense that you can't just take a supplement and hope for the best
The body doesn't work that way and the kidneys are the gatekeepers
If you fail to monitor your labs you are basically asking for calcification
It is pathetic how many people rely on the doctor to tell them what to eat
Read a book on renal nutrition and you would see this is avoidable
The bone loss is just a symptom of a failed lifestyle
Stop complaining about the biology and start fixing the habits
Most of these patients are just lazy with their restrictions
You can't eat processed foods and then wonder why your PTH is screaming
It is a simple equation of input versus output
The science is clear but the discipline is missing
That is why most of these cases end up as a disaster
Jitesh Mohun April 6, 2026
stop whining and just follow the diet rules if u want to live longer
shelley wales April 7, 2026
It is so important to remember that we are all in this together and managing these levels is a journey
Please be kind to yourselves while navigating these complex labs
Grace Lottering April 7, 2026
Big Pharma loves these labels to sell more expensive binders
GOPESH KUMAR April 8, 2026
The irony is that we treat the symptoms but the systemic failure is an inevitable march toward entropy
Most people view the kidneys as filters but they are actually the maestros of the endocrine system
The tragedy is that we only realize the value of the balance once the heart begins to petrify
Timothy Burroughs April 10, 2026
Typical that this is written in a way that makes a simple problem sound like a disaster
In America we have the best clinics to handle this so stop acting like it is some mystery
The labs are just numbers and only a coward fears the calcification
Nathan Kreider April 10, 2026
I know it feels overwhelming but there are so many great ways to manage this with your care team
Just take it one day at a time and keep your head up